Dental implants have a 10-year survival rate of about 96.4%, making them one of the most reliable options for replacing missing teeth. But that success depends heavily on what happens during the healing period, when the titanium implant post fuses with your jawbone in a process called osseointegration.
For most patients, osseointegration takes somewhere between three and six months. That range is wide because healing is not the same for everyone. Your overall health, your habits, the location of the implant, and even your diet all play a role in how quickly (or slowly) your body builds a solid bond around the implant post.
If you are considering dental implants, or if you have already had one placed and want to give yourself the best chance at a smooth recovery, understanding these factors can help you set realistic expectations and take steps to support your healing. Patients dealing with gum disease should also understand how pre-existing oral health conditions factor into the timeline.
How Osseointegration Works and Why It Matters
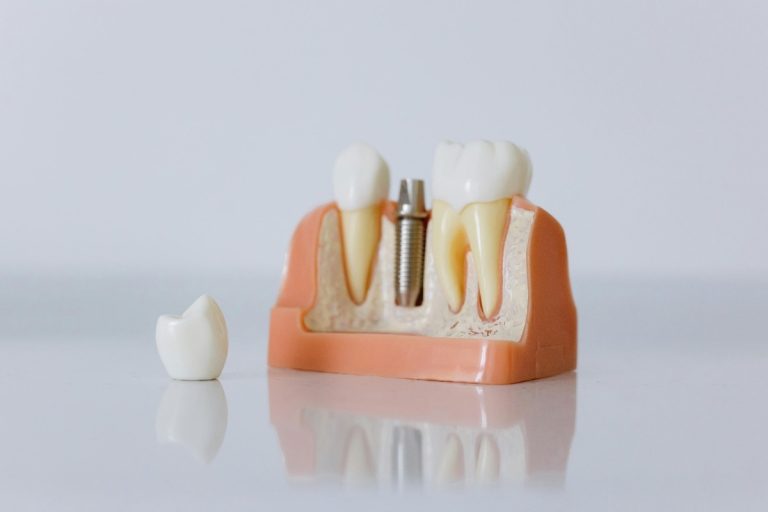
Osseointegration is the biological process where your jawbone grows directly onto the surface of a titanium implant. It is what gives the implant its stability, essentially turning the post into an artificial tooth root that can handle the daily forces of chewing and biting.
The process begins almost immediately after surgery. Your body sends blood cells and growth factors to the surgical site, and new bone tissue begins forming around the implant surface. During the first few weeks, this new bone is immature and relatively soft. Over the following months, the body remodels this tissue into denser, stronger bone that can support a permanent crown or restoration.
If osseointegration does not complete successfully, the implant can loosen and eventually fail. That is why the healing period is so important, and why your dentist will wait until imaging and stability tests confirm solid integration before attaching your final restoration.
Where the Implant Is Placed
One of the biggest factors in healing time is something you cannot control: the location in your mouth where the implant goes.
Upper Jaw vs. Lower Jaw
Lower jaw implants typically integrate in three to four months, while upper jaw implants often need four to six months. The reason comes down to bone density. The lower jaw (mandible) has thicker, denser cortical bone, which gives the implant strong initial stability and a solid foundation for new bone to grip onto. The upper jaw (maxilla) has softer, more porous cancellous bone, which means the biological fusion process simply takes longer.
Bone Quality and Bone Grafting
Your jawbone needs a certain volume and density to hold an implant securely. When either falls short, your dentist may recommend a bone graft before, or sometimes during, implant placement.
Why Bone Density Matters
Denser bone grips the implant tightly from day one, giving it what clinicians call primary stability. Higher primary stability tends to correlate with faster, more predictable osseointegration. Patients with lower bone density, whether from prolonged tooth loss, osteoporosis, or natural anatomy, may experience a slower integration period because the bone around the implant is less compact.
How Bone Grafts Affect the Timeline
A bone graft adds a separate healing phase to the process. It takes a minimum of three months for a dental bone graft to heal, though larger grafts may need nine to twelve months. The type of graft material, the size of the defect, and the location all influence how long healing takes. Simpler socket preservation grafts may heal in three to four months, while more extensive sinus augmentation grafts can take six to twelve months or longer.
Once the graft has matured, Cleveland Clinic recommends placing the implant within six to twelve months, because unused bone grafts gradually lose density over time. If you need a bone graft, your total treatment timeline from graft to final restoration could be anywhere from nine months to over two years.
Smoking and Tobacco Use
Smoking is one of the most well-documented risk factors for implant complications. A 2021 systematic review and meta-analysis that analyzed over 150,000 implants found that implants in smokers had a 140% higher risk of failure compared to non-smokers, with an odds ratio of 2.4.
Nicotine constricts blood vessels, which reduces blood flow to the surgical site. Less blood flow means fewer oxygen and nutrients reaching the area where your bone is trying to fuse with the implant. Smoking also suppresses the function of osteoblasts (the cells that build new bone) and promotes the activity of osteoclasts (cells that break bone down). The result is slower bone formation and a weaker bond between the implant and your jaw.
A meta-analysis published in PLOS ONE that reviewed over 40,000 implants found smokers had roughly double the failure risk compared to non-smokers. The risk also increases with heavier consumption. A separate meta-analysis found that patients who smoke more than 20 cigarettes per day had an even higher failure risk, confirming a dose-response relationship between smoking volume and implant failure.
Most oral surgeons strongly recommend quitting smoking before surgery and remaining smoke-free throughout the healing period. Research suggests ceasing tobacco use at least one week prior to surgery to reverse short-term effects like increased blood viscosity, with longer cessation periods providing additional benefit. After surgery, patients should avoid smoking for at least two months to allow osseointegration to progress through the critical osteoblastic phase.
Do you have questions about your healing timeline? Every patient is different. We can give you a clear, honest look at what to expect based on your health and habits.
Diabetes and Blood Sugar Control
Diabetes does not automatically disqualify you from getting dental implants, but your blood sugar control directly influences how well and how quickly you heal.
A systematic review published in the International Journal of Implant Dentistry found that patients with well-controlled diabetes achieved implant success rates comparable to non-diabetic patients. However, poorly controlled diabetes significantly delays the healing process. A study published in the Journal of Dental Research found that poor glycemic control has been associated with slower implant stabilization and healing, while well-controlled diabetes is generally associated with better outcomes.
High blood sugar impairs your immune response and slows wound healing throughout the body, and your mouth is no exception. Elevated glucose levels reduce the activity of bone-building cells, increase the risk of post-surgical infection, and slow down the formation of new blood vessels at the implant site.
The good news is that with proper glycemic management, diabetic patients can achieve excellent long-term outcomes. If you have diabetes, your dentist will likely coordinate with your physician to ensure your blood sugar is well-managed before scheduling implant surgery.
Medications That Can Slow Healing
Several common medications can interfere with bone remodeling or complicate the surgical healing process.
Bisphosphonates
Bisphosphonates are medications prescribed for osteoporosis that work by slowing the breakdown of bone tissue. While that sounds like it would help implant healing, the process is more nuanced. Osseointegration requires a balance of bone breakdown and bone formation. Bisphosphonates suppress the bone-remodeling cycle, which can interfere with the normal healing sequence. In rare cases, long-term bisphosphonate use is associated with medication-related osteonecrosis of the jaw (MRONJ), a condition where jawbone tissue fails to heal after dental surgery.
Blood Thinners
Medications like warfarin, aspirin, and newer anticoagulants can increase bleeding during and after surgery, which may complicate the early healing process. If you take anticoagulants or antiplatelet medications, your dentist and prescribing clinician should review them before surgery. In many cases these medications are not routinely stopped, but the plan depends on the procedure and your medical risk.
Immunosuppressants and Steroids
Drugs that suppress your immune system, including long-term corticosteroid use and medications taken after organ transplants, can slow wound healing and reduce your body’s ability to fight infection at the implant site.
Always provide your dentist with a complete list of every medication and supplement you take before implant surgery. This is not just a formality. It directly impacts your treatment plan and healing protocol.
Nutrition and Vitamin Deficiencies
What you eat during recovery matters more than most patients realize. Your body needs specific raw materials to build new bone and heal soft tissue, and a poor diet can slow the process considerably.
Vitamin D and Calcium
Vitamin D helps your body absorb calcium, which is the primary mineral in bone tissue. A scoping review in Nutrients found a clear link between severe vitamin D deficiency and increased early implant failure, with deficient patients experiencing an 11.1% early failure rate compared to 2.9% in patients with normal vitamin D levels. Vitamin D supplementation also appeared to counteract marginal bone loss around implants.
If testing shows vitamin D deficiency, your physician or dentist may recommend treatment based on your lab values and overall health.
Protein and Overall Diet
Protein is essential for wound repair and immune function. A diet lacking in protein, vitamin C, and other micronutrients can compromise your body’s healing capacity. In the weeks following surgery, focus on nutrient-dense soft foods: yogurt, eggs, fish, cooked vegetables, smoothies with protein powder, and bone broth are all solid choices.
Concerned about a health condition? Specific medications don’t always stop you from getting implants. We can help you create a safe plan that fits your medical history.
Teeth Grinding and Clenching (Bruxism)
Bruxism, the habitual grinding or clenching of teeth, places excessive mechanical force on dental implants, particularly during the critical osseointegration window when the bond between implant and bone is still forming.
If you grind your teeth, your dentist will likely recommend a custom nightguard to protect the implant during sleep. In some cases, they may also adjust the treatment timeline to allow for a longer unloaded healing period before attaching the final crown.
Oral Hygiene During Recovery
Keeping the surgical site clean is non-negotiable during healing. Bacterial buildup around the implant can cause infection, which can progress to peri-implantitis, a condition where the bone supporting the implant begins to break down.
Your dentist will give you specific post-operative instructions, typically involving gentle brushing around the site, saltwater or antimicrobial rinses, and avoiding vigorous rinsing or spitting for the first 24 to 48 hours. Following these instructions closely is one of the simplest and most effective things you can do to keep your healing on track.
Poor oral hygiene does not just slow healing. It can cause the implant to fail entirely. Treating your recovery like a daily commitment rather than a one-time event makes a measurable difference in outcomes.
What You Can Do to Support Faster Healing
While some factors are outside your control, many are not. Here is what the evidence supports for giving your implant the best chance at a smooth recovery.
Before Surgery
Talk to your dentist about every medication and supplement you take. If you smoke, begin a cessation plan as early as possible. If you have diabetes, work with your physician to optimize your levels. Ask about your vitamin D levels and supplement if needed.
After Surgery
Follow your post-operative instructions exactly. Eat a nutrient-rich, soft-food diet during the first several weeks. Avoid smoking, drinking through a straw, and any activity that creates suction in your mouth. Attend every follow-up appointment so your dentist can monitor the integration process.
Throughout the Process
Keep up with gentle oral hygiene. If you grind your teeth, wear your nightguard consistently. Avoid chewing hard or crunchy foods on the implant side until your dentist clears you.
The healing period requires patience, but it is the foundation for an implant that can last decades. If you have questions about your specific healing timeline, the team at Englewood Dental can evaluate your individual situation and walk you through what to expect.
Ready to start? Healing takes time, but the results are worth it. If you are in the Englewood area, let’s see if dental implants are the right choice for you.
Frequently Asked Questions
Can I speed up dental implant healing?
You cannot significantly speed up the biological process of osseointegration, but you can avoid slowing it down. Not smoking, maintaining good blood sugar control, eating a nutrient-rich diet, and following your dentist’s post-operative instructions all contribute to healing that stays on schedule rather than falling behind.
Does smoking really affect dental implant success?
Yes. Research shows that smokers have roughly double the risk of implant failure compared to non-smokers. Nicotine restricts blood flow, suppresses bone-forming cells, and increases the risk of infection at the surgical site.
Are dental implants safe for people with diabetes?
Dental implants can be very successful for diabetic patients, provided blood sugar is well-controlled. Patients with controlled diabetes tend to achieve outcomes similar to non-diabetic patients. Poorly controlled diabetes can extend healing time and increase the risk of complications.
What happens if my dental implant does not heal properly?
If osseointegration fails, the implant will become loose and may need to be removed. In many cases, your dentist can place a new implant after the site has healed, sometimes with a bone graft to rebuild the area. Early detection through regular follow-up visits improves the chances of catching and addressing problems before the implant is lost.