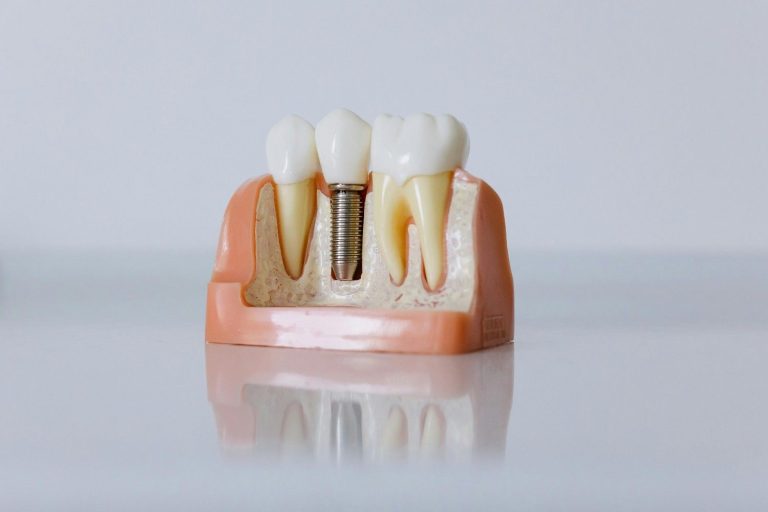
Yes, patients with gum disease can get dental implants, but only after the infection is properly treated and controlled. Active periodontal disease must be resolved before implant placement to reduce the risk of failure or peri-implantitis. With appropriate periodontal therapy, bone support evaluation, and careful treatment planning, many patients with a history of gum disease can successfully receive long-lasting implants.
Wondering if you’re a candidate?
Dental implants are widely recognized as the gold standard for replacing missing teeth due to their durability, natural feel, and ability to preserve jawbone integrity. Yet, for patients with gum disease, medically known as periodontal disease, the journey to implant success raises critical questions: Can you get dental implants with gum disease? What treatments are necessary? How does gum health influence long-term outcomes?
What Is Gum Disease and Why It Matters for Dental Implants
Gum disease starts as gingivitis, inflammation of the gums, and can progress into periodontitis, where the infection erodes the gum tissue and the underlying bone that supports the teeth. In advanced stages, the disease causes bone loss and increases the risk of losing teeth altogether.
Dental implants rely on a robust foundation of healthy gum tissue and jawbone. When active periodontal disease is present, this foundation is compromised, which can reduce the chances of implant integration and stability.
Can Patients With Gum Disease Get Dental Implants?
Yes, but only after gum disease is treated and controlled. Active periodontal infection must be resolved before implant placement can be considered. Placing an implant into an infected or inflamed site significantly increases the risk of implant failure and complications like peri-implantitis, an infection affecting the tissues around an implant.
Gum disease does not permanently disqualify patients from dental implant surgery, but successful implants demand a healthy oral environment free of active infection.
Not sure if your gum health qualifies you for implants? A detailed exam can give you clear answers.
Find Out If You’re a Candidate
Step-by-Step Guide: Preparing for Dental Implants With Gum Disease
1. Comprehensive Periodontal Evaluation
Before treatment begins, your dentist will conduct detailed periodontal charting to assess gum pocket depths and bone levels. This helps determine the severity of gum disease and guides treatment planning.
2. Gum Disease Treatment
Initial treatment includes scaling and root planing, which removes plaque and tartar below the gum line and helps the gum tissue heal. More advanced periodontal therapy may involve surgical intervention, laser procedures, or localized antibiotics.
3. Healing and Reassessment
Once gum disease is controlled, your dental team will reassess gum and bone health. This waiting period ensures tissues are stable and ready to support new implant posts.
4. Bone Grafting (If Needed)
Because gum disease often leads to jawbone loss, bone grafting may be necessary to rebuild sufficient bone density that can support implant osseointegration (the biological bonding of the implant to bone).
5. Dental Implant Placement
With healthy gums and adequate bone support, your dentist can place implants safely. Proper healing time and careful surgical technique maximize chances of long-term success.
Why Gum Health Determines Implant Success
Healthy gums act like a seal around your teeth and implants, protecting the deeper structures from bacteria. When periodontal disease is active and unchecked, it increases the risk of bacterial invasion around an implant, compromising healing and long-term success.
Clinical research has long established that soft tissue health is as crucial as bone integration for implant longevity, a principle that has guided implant protocols for decades and continues to be reinforced by ongoing peer-reviewed literature.
Have a history of gum disease? Start with a comprehensive periodontal and implant evaluation.
Schedule Your Implant & Gum Health Consultation
Advanced Implant Options for Patients With Severe Gum Disease
For patients with extensive bone loss or full-arch tooth loss caused by periodontal disease, modern solutions such as All-on-4 and zygomatic implants may be viable options in appropriate cases.
All-on-4: The All-on-4 technique replaces an entire dental arch using four implants, with the posterior implants angled to utilize available bone and reduce, though not always eliminate, the need for bone grafting. While this approach can be advantageous for patients with moderate bone loss, some patients may still require grafting, and candidacy must be assessed on an individual basis.
Zygomatic implants: In cases where the upper jawbone is severely diminished, zygomatic implants anchor into the cheekbone (zygomatic bone) rather than the jaw, bypassing the need for significant bone grafting in the upper arch. It is important to note that zygomatic implants are indicated exclusively for the upper jaw and are a highly specialized procedure performed only by specially trained surgeons at select clinical centers. They are not a routine option and require careful patient selection.
In cases where the upper jawbone is severely diminished, zygomatic implants anchor into the cheekbone (zygomatic bone) instead of the jaw, bypassing compromised bone.
How to Keep Implants Healthy After Placement
Once dental implants are placed, maintaining gum health is essential to prevent peri-implantitis, a condition similar to periodontal disease but specific to implants. Good habits include brushing twice daily, flossing or using interdental brushes, and seeing your dental professional regularly for cleanings and monitoring.
Lifestyle factors such as quitting smoking and controlling systemic conditions like diabetes also contribute to implant longevity.
Dental Implants, Gum Health, and Long-Term Oral Care
Successful dental implant treatment is not only about replacing a missing tooth but also about building a foundation for long-term oral health. Modern dental implants function like a natural tooth root, are placed into the jawbone, and help prevent bone loss after tooth loss. Through osseointegration, the implant fuses with bone, providing stability similar to natural teeth.
Peer-reviewed literature consistently reports dental implant success rates in the range of 90–96% over 10-year follow-up periods, with outcomes varying based on patient health, bone quality, oral hygiene, and professional monitoring. Patients with well-controlled gum health and regular professional care tend to fall toward the higher end of this range.
Many patients underestimate how closely gum disease and implant success are linked. Conditions like periodontitis can cause gum irritation, bone loss, and inflammation that jeopardize implant placement.
That is why dentists increasingly recommend a personalized care and treatment plan that may include periodontal therapy, bone grafting, and sometimes sedation for anxious patients.
From a preventive standpoint, simple habits such as daily brushing, flossing, and routine dental visits help detect dental issues early, including cavities, plaque buildup, and signs of gum disease.
The World Health Organization highlights that good oral hygiene and preventive dentistry play a major role in long-term oral health and overall well-being. This is particularly important for patients choosing advanced solutions like implants or transitioning from a denture to fixed restorations.
Ultimately, patients choose dental implants not only for aesthetics but also for improved comfort and long-term oral health.
With a clear care plan, attention to teeth and gums, and guidance from experienced dental professionals, implants remain a safe and evidence-supported solution for restoring a healthy smile.
Gum disease doesn’t automatically disqualify you. Proper planning makes all the difference.
Frequently Asked Questions (FAQs)
Can I get dental implants if my gum disease is mild?
Yes. Mild gum disease (gingivitis) is typically treatable with deep cleaning and improved oral hygiene before implant placement.
Does gum disease have to be fully healed before implants?
Yes, implants should only be placed after active periodontal infection has been controlled to avoid complications and promote healing.
What happens if gum disease returns after implants?
If gum disease recurs, patients are at higher risk for peri-implantitis, which can jeopardize implant stability if not managed promptly.
How long is the healing time after treating gum disease before implant surgery?
Healing time varies based on severity but generally includes several weeks of monitoring to ensure tissue stability before implant placement.
Conclusion
Patients with gum disease no longer face an automatic barrier to dental implants. The key to success lies in comprehensive periodontal treatment, diligent oral care, and careful planning that ensures gums and bone are healthy enough to support implants.
Even individuals with a history of periodontal disease can achieve stable, long-lasting implant-supported smiles in 2025 and beyond. Schedule Your Implant Consultation Today at Englewood Dental Clinic.